
Scott and Paul May with a photo of their parents. Their father, Bill May, was killed by his roommate at a care home for patients with complex behavioural issues.
(CHARLOTTE HELSTON / iNFOnews.ca)
August 23, 2016 - 9:00 PM
“WE’RE LOOKING FOR SOME FEET HELD TO THE FIRE FOR CHANGE BECAUSE THIS IS BECOMING A BIGGER ISSUE”
VERNON - The families of two elderly dementia patients who died in separate care home attacks are speaking out about their frustrations that more isn’t being done to prevent similar deaths.
It’s been three years since Bill May, an 85-year-old resident at the Polson Special Care Unit in Vernon was killed by his delusional roommate. It has also been well over three years since Jack Shippobotham, a 79-year-old dementia patient in Kamloops, died after being attacked by a fellow resident.
Now, the men’s families are sharing their frustrations that the one positive thing they hoped would result of the tragedies — preventing a similar death — is not being taken more seriously.
Bill May’s sons Scott and Paul say they spoke with representatives from Interior Health at their own initiative following the August 2013 incident to find out what the health authority planned to do to prevent another death.
Roughly six months later, in January 2014, they met with Interior Health officials and were shown the results of a ‘quality improvement review’ intended to enhance care and safety for seniors with ‘complex behaviours.’
Among a series of 18 actions from the review, Interior Health said it was going to create a special working group, develop a process for reaching out to families, make modifications to enhance safety ‘where appropriate’, and ‘where feasible, over time’ work on getting more single patient rooms.
Paul and Scott May say the recommendations are vague and lack any concrete change.
“It seemed they were doing the stuff easily improved upon, like speaking with family," Scott says. "Not so much the prevention stuff.”
“What actual physical procedural changes are happening?” Paul adds.

Bill May with his wife Bonnie.
Image Credit: Contributed
At their meeting with Interior Health, they suggested video or audio monitoring systems be installed in the rooms. In their father’s case, night shift staff did not become aware of the assault until they heard a noise coming from his room. When they arrived, they found May lying at the foot of his bed while his roommate stood over him with a blood-covered shelf. The coroner’s report found that May died of multiple blunt force trauma.
And it wasn’t the first time May was injured at that care home, which is designed for patients with complex behavioural issues and advanced dementia. His sons say on various occasions when they went to see him he was missing a tooth, had a black eye, what may have been a broken nose, and his glasses were broken twice. They feel better monitoring could help with early intervention of such altercations, and maybe save a life.
“You can’t say for certain, but if someone heard a scuffle (on a monitor) before they heard it through a door, maybe you could get there in time to stop it,” Scott says, adding Interior Health cited privacy concerns with the installation of monitors.
They’ve heard nothing further from Interior Health since that meeting, and say the actions listed in the report won’t amount to any meaningful change.
“It feels more and more like lip service and pacifying to me to say ‘look, we’ve done something,’” Scott says.
iNFOnews.ca contacted Interior Health on Friday, Aug. 19 to find out what, if any, actions have been implemented from the January 2014 report, but did not receive a response before deadline on Aug. 23.
In November 2013, when iNFOnews.ca requested more information about an internal review conducted by Interior Health on the specific incident that led to May's death, a spokesperson said few, if any, of the findings could be released for privacy reasons.
The May family is calling for action and more transparency from the health authority about what it is doing to make care homes safer.
“If I was in charge of a place that had these kinds of incidents, I would be looking for the physical changes — what can I do, not what can I study,” Paul says. “I always wanted us to be on the same side — it’s not about pointing fingers. We’re all on the same page, no one wants this to happen again.”
The family is also frustrated with the results of a recently released coroner’s report that includes no recommendations to prevent a similar death.
“I’d like to have seen a coroner’s inquest, because that would make it very public,” Scott says. “I think enough of these incidents are happening, and foreseeably more of them coming, and it’s totally appropriate to have an inquest.”
Barb McLintock, with the B.C. Coroners Service, says the chief coroner weighs all inquest requests carefully, and makes decisions based on public interest, public risk, and the need for public review of evidence.
"In cases where the circumstances are clearly established and not in issue, and where more general issues are being reviewed by another body, an inquest may not be necessary,” McLintock says.
LONG WAIT FOR ANSWERS
The daughter of Jack Shippobotham shares the May family’s frustration. Moneca Jantzen has been vocal in the media and online about the need for better monitoring, private rooms, and locks that allow residents to leave their rooms but prevent other patients from wandering in and getting into altercations, as was the case with her father.
“The Interior Health Authority and the private facilities have to stop doing the bare minimum and take better care of our elders in these facilities. It breaks my heart every time it happens,” Jantzen says, pointing to the 2015 death of another Kamloops senior, Emily Houston, who also died after being assaulted by a patient.
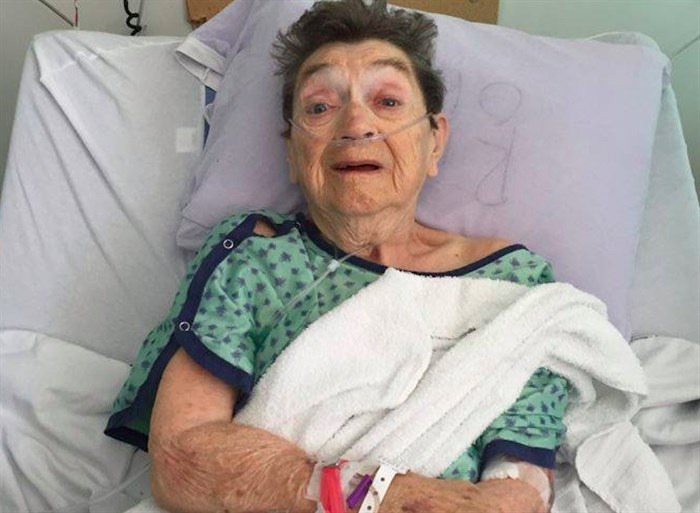
Houston, after she was assaulted by a fellow care home resident in July 2015.
Image Credit: contributed
After more than three years, Jantzen has still not received the coroner’s report for her father.
“Three years is a ridiculous amount of time to wait for what will likely amount to very few answers if the May-Furman case is any indication of what gets shared,” she says.
Still, she hopes the report will be released soon so her family can move on with at least some official answers. She’s also received unofficial information from the investigating coroner that two recommendations were made in relation to her father’s death. Jantzen hopes those recommendations will be on the report released to the public and are “not removed during the review process by the powers that be.”
The coroners service expects to release the Shippobotham report in the next few weeks, and McLintock says they recognize the investigations in both cases have taken longer than usual to conclude.
“Some of this is due to other investigative demands but the coroner also spent considerable time gathering information about the growing problem of resident-on-resident aggression in facilities housing patients suffering from dementia, and considering options for concluding the investigations," McLintock says. "However, we recognized that cases which result in death are a very small proportion of the total number of cases of this type of aggression. We were pleased, therefore, when we learned that the Seniors’ Advocate had begun a serious study of this problem as we believe hers is the agency with the mandate and expertise to review these issues more comprehensively."
HUNDREDS OF INCIDENTS OF CARE HOME AGGRESSION
In June of this year, the B.C. seniors advocate came out with recommendations aimed at preventing violence in care homes. Her investigation found nine deaths related to resident aggression since 2012, and more than 422 incidents in which residents were harmed over a one year period.
Her report concluded that facilities with the most incidents of aggression tended to be those with patients experiencing complex care needs and behavioural issues. Despite having higher care needs, those facilities actually had a lower amount of funded care hours.
“While we would expect more complex residents translates to more care hours, unfortunately we don’t see this and this concerns me,” advocate Isobel Mackenzie said. “Even in facilities with the most complex residents and highest incidence of aggression some fall below the minimum provincial guideline of an average of 3.36 care hours per resident per day and we must look more closely at what appropriate care hours are in these facilities.”
Mackenzie recommended more training for staff and called on facilities to adopt strategies and design features that are known to be effective in mitigating aggressive behaviours. Her report did not specifically call for higher staffing levels, but indicated a need to further explore the adequacy of staffing for residents with complex needs.
But after three years of reports and studies, the families of those lost in care home attacks are demanding action now.
“We’re looking for some feet held to the fire for change because this is becoming a bigger issue,” Scott May says.
Families themselves may well have to play a part in holding feet to fire. Jantzen encourages anyone who has a loved one in a care home to insist that facilities report on incidents fully and truthfully so lessons can be learned.
“We can't fix what isn't working if we don't identify the problems. Facilities that prefer to sweep these incidents under the proverbial carpet will never be held accountable and will certainly never improve their levels of care if the reporting system isn't working from the get go,” Jantzen says.
To contact a reporter for this story, email Charlotte Helston or call 250-309-5230 or email the editor. You can also submit photos, videos or news tips to the newsroom and be entered to win a monthly prize draw.
We welcome your comments and opinions on our stories but play nice. We won't censor or delete comments unless they contain off-topic statements or links, unnecessary vulgarity, false facts, spam or obviously fake profiles. If you have any concerns about what you see in comments, email the editor in the link above.
News from © iNFOnews, 2016