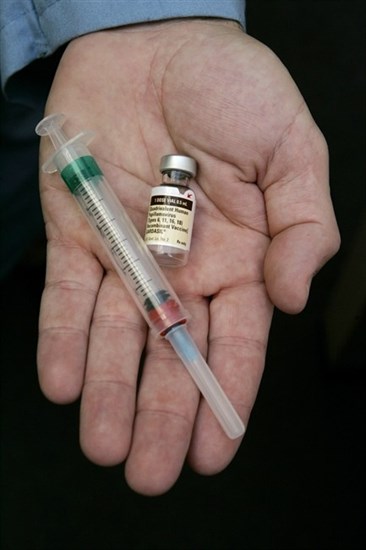
A doctor holds the human papillomavirus (HPV) vaccine Gardiasil in his hand at his Chicago office in this Aug. 28, 2006 file photo. A new study suggests there is more support for HPV vaccination than one might expect, given the controversies that dogged the vaccine programs in their early days.
Image Credit: THE CANADIAN PRESS/AP/Charles Rex Arbogast, File
June 12, 2015 - 7:02 AM
TORONTO - There may be more support for HPV vaccination than you might expect, given the controversies that dogged the vaccine programs in their early days, a new study suggests.
But it also found misinformation about the vaccines abounds. And it gives public health officials clues as to how to reframe the debate about vaccines that protect against cancer-causing human papillomaviruses.
The research was done by scientists at Public Health Ontario who analyzed comments posted online in response to Canadian newspaper articles on HPV vaccine. It was published in the online journal PLoS One.
While there was lukewarm response to the vaccine in Ontario when the provincial program started in 2007, 80 per cent of Grade 8 girls were vaccinated against HPV in 2012-13, the most recent year for which data are available. (Three provinces currently or will soon also offer the vaccine to boys: Prince Edward Island, Alberta and Nova Scotia.)
"We still have a way to go. There are misperceptions," said senior author Dr. Shelley Deeks, the Ontario agency's medical director for immunization and vaccine preventable disease.
"And we need to focus on this vaccine as an anti-cancer vaccine, aside from the ... anti-STD type of promotions."
STD is short for sexually transmitted disease.
For the study, the authors searched for HPV vaccine-related articles published on the websites of Canadian newspapers in 2012. They found 71 articles which generated 3,073 reader comments posted by 1,198 people.
Nearly 53 per cent of the comments were favourable toward the vaccine, which Deeks admitted was a surprise.
But about a third of commenters posted negative remarks, questioning the safety of the vaccine, the motives of pharmaceutical companies and government and whether school-aged children were too young to be vaccinated against viruses that are sexually transmitted.
Often the negative comments contained some truth — just not the whole story, Deeks said.
For instance, some noted most people clear HPV infection on their own. But a small number don't and they are the people who go on to develop cervical cancer, penile and anal cancers and other forms of the disease. And it is currently not possible to predict who will and who won't.
"There's a kernel of truth. But it's just not the whole truth. And it's the important piece that they're missing."
There are two HPV vaccines — Gardasil, made by Merck, and Cervarix, made by GSK. Both protect against infection with human papillomaviruses that cause cervical cancer; Gardasil also protects against HPV viruses that cause genital warts.
People contract these viruses through sexual activity. It is estimated that at least 70 per cent of sexually active people are infected at least once in their lifetimes. Studies have shown infection often happens within the first couple of years after a person becomes sexually active.
Because of that — and the fact that younger immune systems respond better to these vaccines — provincial and territorial programs deliver these vaccines early. Several jurisdictions start in Grade 4, while others start in Grades 5 through 8.
But vaccinating at these ages triggered concern in some quarters that the vaccine would give girls licence to have sex at an earlier age.
In some locations Roman Catholic school boards initially refused to let public health departments set up clinics in their schools. One such ban, by Calgary's Catholic board, was lifted during the year the researchers were studying.
Deeks said the comments suggest that focusing more attention on the cancer prevention qualities of the vaccine might help public health overcome parental concerns.
Eve Dube of Quebec's public health agency agreed. A medical anthropologist, Dube noted that hepatitis B vaccine has not experienced the same resistance.
That vaccine protects against a virus that can cause liver cancer. It is given either in infancy or in Grades 4 through 7, depending on the province or territory. Hepatitis B can also be transmitted through sex.
Dube, who has been involved in similar studies to this one, suggested assessing comment boards can give public health authorities a different and potentially broader view of public perceptions of vaccines.
"It gives you a more qualitative understanding of what people think," she said.
News from © The Canadian Press, 2015