
Vernon resident Allison Kooijman has spent the last five years of her life seeking justice for an erroneous cancer diagnosis.
(CHARLOTTE HELSTON / iNFOnews.ca)
March 30, 2017 - 8:00 PM
VERNON - Most people would be relieved to hear they had a false positive test result for cancer. Not Allison Kooijman.
She didn’t find out until after she’d already had a major surgery that removed 16 perfectly healthy lymph nodes removed from the left side of her neck. Her spinal accessory nerve was damaged in the process, leaving her feeling as if “someone is hanging off my shoulder blade all the time.”
Interior Health acknowledges it was an error, and a B.C. Supreme Court Judge found two of the pathologists breached the standard of care, but Kooijman, who is now on disability, won’t see any compensation. Instead, it cost her dearly in expenses, time and anxiety, a career as a nurse and current and future earnings.
When you get injured in a car accident, you can file a claim with ICBC. If you get hurt on the job, there’s WorkSafe B.C. But, as Kooijman and other patients have learned, the only way you can seek compensation in B.C. for an injury of medical malpractice is by going to court. And when you do that, not only do you have to meet a very high burden of proof, you’re up against the Canadian Medical Protective Association — a massively endowed, partially taxpayer-subsidized defence for doctors that is awfully hard to beat.
FALSE POSITIVE CANCER DIAGNOSIS
Kooijman traces the faint line that runs from her left ear, down to her left clavicle, across her neck and back up the other side.
“I call it my Frankenstein scar,” she says. “I was opened up like a book.”
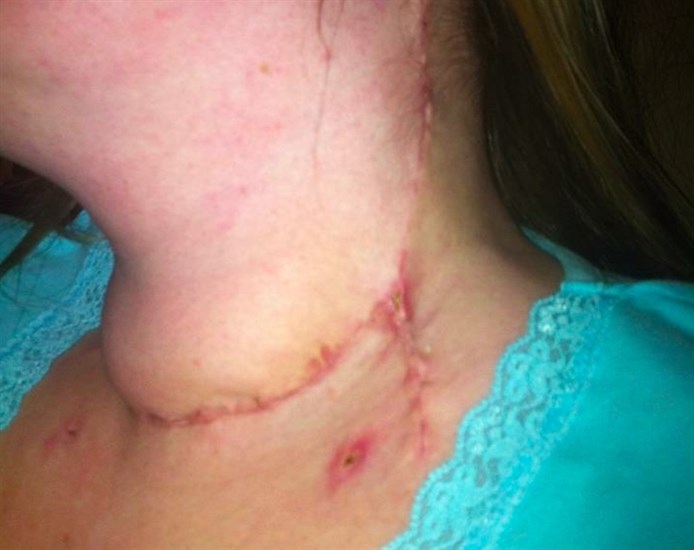
Kooijman describes the surgery as having her neck "opened up like a book."
Image Credit: Submitted
In February 2012, Kooijman was scheduled for a right side neck dissection to remove a cancerous lymph node. She’d already been diagnosed and treated for thyroid cancer back in 2010, but a recent check-up showed it wasn’t gone.
During a pre-surgery visit with her doctor, Kooijman thought to point out some nodes on the other side of her neck — the left — that she’d been aware of since 2007 when she had mono. Having already been through cancer treatment once, she didn’t want anything to be missed this time around.
While the surgeon wasn’t particularly concerned about the other nodes, he ordered a biopsy to find out for sure. Roughly two weeks before her surgery, Kooijman had the left lymph nodes biopsied. The results came back positive for papillary thyroid cancer — the ‘best cancer to have if you are unlucky enough to have cancer’ Kooijman was told.
Now, instead of a right-side-only neck dissection, she was now having a full, bilateral dissection.
Have you undergone a similar struggle? Contact reporter Charlotte Helston
“You get this report, and you trust it,” Kooijman says. “At that point in time I’m ready to go. I’m like ‘this is what I’m being told to do, this is the information I’ve been given, let’s just get this nightmare over with.’”
It wasn’t until after the surgery and the 30 removed lymph nodes were sent to the lab for more testing that Kooijman found out the pathology report was wrong about the nodes on the left side of her neck. While one of 14 lymph nodes on the right side came back malignant, all 16 on the left side came back benign.
The whole left side dissection was unnecessary.
Medical notes from the time show doctors were confounded by the results.
“At this point it is unclear to me why there was no metastic disease identified in the left neck where 16 lymph nodes were removed,” the surgeon says in medical notes from March 1, 2012.
The samples were retested, and again came back benign. On March 28, 2012 the surgeon stated he has “been reassured that this will be brought to the attention of the head of the IHA Pathology Department.”
Kooijman, meanwhile, was trying to get her life back. In between surgeries, she became a nurse and was eager to start her career. But she didn’t return to work for long. Her spinal accessory nerve on the left side was damaged in the surgery, which, along with a significant amount of muscle and tissue that was removed, has left her with constant pain, migraines and fatigue.
TWICE DISSECTED
Kooijman went under the microscope again in 2016. This time though, it was lawyers and a judge — not doctors — doing the dissecting.
“I felt that I was so hurt, and the quality of my life had changed so dramatically…. There was no doubt in my mind that something should be sorted out, that I should be compensated,” Kooijman says.
A law firm that felt strongly about her case took her on a contingency basis, and the case went to trial in Vancouver Supreme Court April 4. An expert pathologist and an expert oncological surgeon from Ontario testified in support of Kooijman’s claim.
On Dec. 12, 2016, the judge gave his decision: two of the three pathologists who reviewed Kooijman’s biopsy breached their duties of care, however the plaintiff would have opted for the surgery anyway. Case dismissed.
According to Paul McGivern, a medical malpractice lawyer based in Vancouver, this is where many cases fall apart and is one of the reasons why he counsels clients to think long and hard about suing.
“Once you prove negligence, you have to prove the negligence actually caused the harm,” McGivern says.
In Kooijman’s case, when the pathologists took a second look at the slides, they changed their findings from a positive diagnosis to, as one put it, ‘barely adequate; suspicious but not diagnostic for PTC; suggest rebiopsy’ to, as another put it: ‘at the least highly suspicious’ of malignancy. This was a key factor at trial, because the judge concluded even if Kooijman was given this information at the outset, she would “more likely than not” have opted for the same surgery.
“Causation is one of the hardest parts of a malpractice claim,” McGivern says. “The defence knows it is by far the toughest part to get past.”
He would know; he spent 17 years working for the Canadian Medical Protective Association before moving to represent patients. Now, he runs one of very few practices devoted to the highly technical and specialized field of medical malpractice.
The CMPA, on the other hand, “has a group of lawyers who do this 24/7.” They also have roughly $3.5 billion in assets to draw on. According to an annual report for 2015, the most recent numbers that are readily available, the association commenced 166 legal actions in B.C. and Alberta that year. Most were either abandoned (90) or settled (69), but six went to trial. Of those, five were won by the association. There was just a single case where a plaintiff walked away successful.
“I make it my practice to tell people about what these cases involve right up front, because they need to know what kind of thing they’re up against,” McGivern says.
But, patients seeking some form of compensation to make up for things like lost wages and loss of future earnings, it’s the only choice.
“In terms of compensation, it’s the only game in town,” he says.
In a case that shares some similarities to Kooijman's, a former Armstrong woman sued doctors and Interior Health after her husband died of cancer. Eric Nolting went for a check-up in 2012 and learned he was never told about the test results of a mole removed five years earlier, in 2007. The mole tested positive for malignant melanoma yet there was no follow up call, according to the notice of claim. He died of cancer Dec. 4, 2012, at age 38. The lawsuit is ongoing but Shannon Nolting, Eric's wife and the plaintiff in that case, is up against the same challenges — the medical defence fund.
The CMPA is self-described as a ‘mutual defence association’ governed by a council of physicians. Doctors themselves pay a membership, but those fees are heavily subsidized by taxpayers. In 2016, the B.C. government paid $23,900,000 into the Canadian Medical Protective Association rebate program.
In a sense, when you sue for medical malpractice, not only are you paying your legal costs, but technically you are paying a portion of the doctor’s as well.
Take compensation out of the equation, and there are other steps patients can take, McGivern says.
“I’ve had a lot of people over the years say ‘I want to make sure this never happens to anyone else.’ In circumstances like that, if all you want is for someone to be called up on the carpet, a better option is going to the College of Physicians or the hospital review board,” McGivern says. “At least you have the hope that at the end of the day, the physician’s conduct will be reviewed by his or her peers and maybe they will learn something.”
MEDICAL SYSTEM OPEN TO HUMAN ERROR
Kooijman is clear: She does not want this to happen to anyone else. Speaking publicly now won’t change what happened to her. The reason she shares her story is to expose the difficulties of the system, and hopefully, to help the next patient.
Before suing, she took her case to both the College of Physicians and Interior Health. The college sent her a letter stating the pathologists met the standard of care. The hospital arranged a patient quality care meeting. But, unfortunately for everyone involved, mistakes will happen again.
In the words of Interior Health’s discipline head of cyto-pathology: “nothing is ever 100 per cent.”
Dr. Balazs Gerloczy says cyto-pathology is a fairly subjective science and while pathologists are highly trained and regulated, errors in interpretation occur about one to five per cent of cases.
“These are not all major errors, we must emphasize,” Gerloczy says. “They are predominantly minor errors that may cause anxiety for the patient, or repeat testing, but no harm.”
“Unfortunately there is the rare case, less than one per cent, that are major errors, such as in this particular case.”
Knowing mistakes can and do happen is why the health authority has mechanisms in place to reduce the likelihood of a major misdiagnosis being missed. For starters, Interior Health reviews roughly ten per cent of all specimens on a monthly basis. For perspective, last year approximately 115,000 specimens were reviewed in Interior Health— more if you count Kamloops, which operates slightly differently.
“It’s very tedious and time consuming,” Gerloczy says.
There’s also a targeted review of slides that are, by nature, more likely to lead to an erroneous interpretation. Pathologists also conduct peer reviews to get another expert’s opinion. The goal, of course, is to catch the mistake before a patient is treated.
“All the measures of quality assurance were followed in this case. Unfortunately, even with that the mistake happened,” Gerloczy says of Kooijman’s case.
He says such cases are ‘devastating’ to pathologists who treat each slide “as if it was our mother’s specimen, our sister’s specimen, our daughter’s specimen.”
“When there’s a major error I can tell you those will stay with us forever. Those are the best ways of reminding us not not make that kind of mistake again,” he says. “I am very sorry for what happened to this patient. It’s a very unfortunate case, and unfortunate outcome. I can say that we will remember this case.”
Kooijman doesn’t blame her doctors. She understands that mistakes happen, and she was one of those mistakes.
“What’s bigger for me now is that I’m concerned about what happens to the next person. I’ve seen and struggled through the last five years of watching this go to trial, and the environment that comes with that, and the difficulty that patients have. These are generally very vulnerable people. They’re sick, they’re hurt, and I’d like to see something change. I’d like to see an environment where patients and doctors can talk about errors without litigation, and I’d like to see a system put in place to take care of people after something like this happens.”
To contact a reporter for this story, email Charlotte Helston or call 250-309-5230 or email the editor. You can also submit photos, videos or news tips to the newsroom and be entered to win a monthly prize draw.
We welcome your comments and opinions on our stories but play nice. We won't censor or delete comments unless they contain off-topic statements or links, unnecessary vulgarity, false facts, spam or obviously fake profiles. If you have any concerns about what you see in comments, email the editor in the link above.
News from © iNFOnews, 2017